The Affordable Care Act (ACA) Section 1332 waiver provisions allows states to modify the baseline of the ACA to fit local circumstances. These waivers must meet four criteria. Coverage has to be as good, as affordable, for at least as many people and cost the federal government no more money. The, by far, most common type of waiver that has been filed and approved has been a reinsurance waiver. Reinsurance, in the ACA context, means that a non-premium source of revenue is used to pay a chunk of claims. This has the effect of lowering gross premiums which lowers subsidized premiums. The lower subsidized premiums means the federal government spends less on premium subsidies. Those incremental funds are then effectively shifted to non-subsidized buyers.
This complex plumbing is needed because states have a strong policy and political incentive to minimize the pain of non-subsidized buyers as I outlined in a Health Affairs article from 2019.
States have three primary options for reducing premiums for households ineligible for federal APTCs: direct subsidization, indirect subsidization, and endorsement of parallel markets…
Indirect subsidization through state-based reinsurance programs authorized by Section 1332 waivers is another way to enhance plan affordability.
These waivers make a lot less sense in the ARPA/IRA subsidy environment. Everyone can not purchase a baseline silver plan for no more than 8.5% of their income. Coleman Drake and I made this point in JAMA Health Forums:
The ARP’s enhanced premium subsidies undercut the logic of state-based reinsurance programs by capping benchmark marketplace premiums at 8.5% of household income for families with incomes above 400% of the federal poverty level. Capping premiums means that premium levels no longer determine the affordability of marketplace plans for these enrollees….
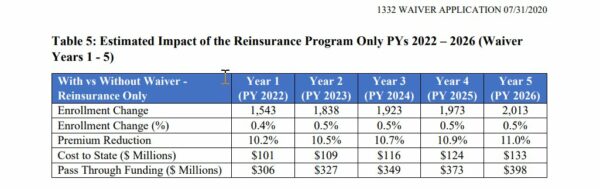
Reinsurance was mostly a solution to a problem that ARPA/IRA has temporarily solved. However, there is little research on how effective reinsurance is at extending coverage. I’m going to look at the Georgia waiver submission packet from 2020 as it is a big waiver with an easy to pull out table. My question is how much does the state spend to buy an extra covered life. I’m using only their projections so if they are too optimistic, the projected price will be too low compared to reality and vice versa.
In the first year of the projected waiver, the state anticipates spending $65,400 to insure one additional person through the reinsurance program. By year 5 (2026), the state thinks it will spend just over $66,000 per incremental covered life.
Is this cost effective?
Maybe?
We traditionally value a quality adjusted life year in the United States at between $50,000 to $125,000. $100,000 per QALY is a reasonable threshold for commercial insurance before insurers start getting antsy about paying.
If we take $100,000 as the QALY threshold, then each newly insured individual needs to gain about 0.70 QALY per newly covered life year.
THAT IS A LOT!
I’m not sure what I think.
I think the Goldin, Lurie, McCubbin’s population is not quite the right population to generalize to. I think their studied population is a bit poorer (<400% FPL) and not as actively health insurance seeking. My prior is the Georgia incremental insured population is healthier with lower mortality risks than the Goldin, Lurie, McCubbin population.
I think that this is an active question that as far as I know, no one is looking at. We should figure this out. The answer might not matter all that much on the policy side as policy makers frequently have objectives that are not constrained only to cost-effective life maximization. Political concerns such as satisfying an aggrieved, well organized and well connected constituency can often become a priority even if the intervention may or may not be cost-effective depending on the underlying policy analysis assumptions.

Lobo
Politics is satisfying an aggrieved, well organized, well connected constituency and making progress for marginalized voices. It is an “and” not an “or”. Given that how do we make the best of it?