The Notice for Benefits and Payment Parameters (NBPP) is the Center for Medicare and Medicaid Services (CMS) annual playbook for running Healthcare.gov. Most of it is fairly boring mechanical changes to risk adjustment but there are always some significant policy changes in it.
One of the quiet policy changes is the expansion of a hardship exemption for individuals who live in counties where there is either no insurers or a single insurer offering coverage. Here is the language from the fact sheet:
CMS also issued new guidance today expanding hardship exemptions. Under this hardship exemption guidance, individuals who live in counties with no issuers or only one issuer, will now qualify for a hardship exemption from paying the Affordable Care Act’s penalty for not having coverage.
The no insurer part makes sense, it formalizes the procedure of what could be done in a bare county. I think pretty much every health wonk in the country has thought that if a county has no insurers, a hardship exemption would be granted on either automatic affordability grounds(divide by zero error) or on Secretary’s discretion.
The interesting part was the extension of a hardship exemption to single carrier counties. About a quarter of enrollees in 2018 were in single carrier regions. This was odd. An exemption allows an individual to not pay the individual mandate penalty. The individual mandate penalty zeroes out but is not eliminated on January 1, 2019.
I originally did not think this was a big deal:
This makes me lean towards thinking that these two exemptions are primarily messaging rules and not rules with significant pragmatic impact.
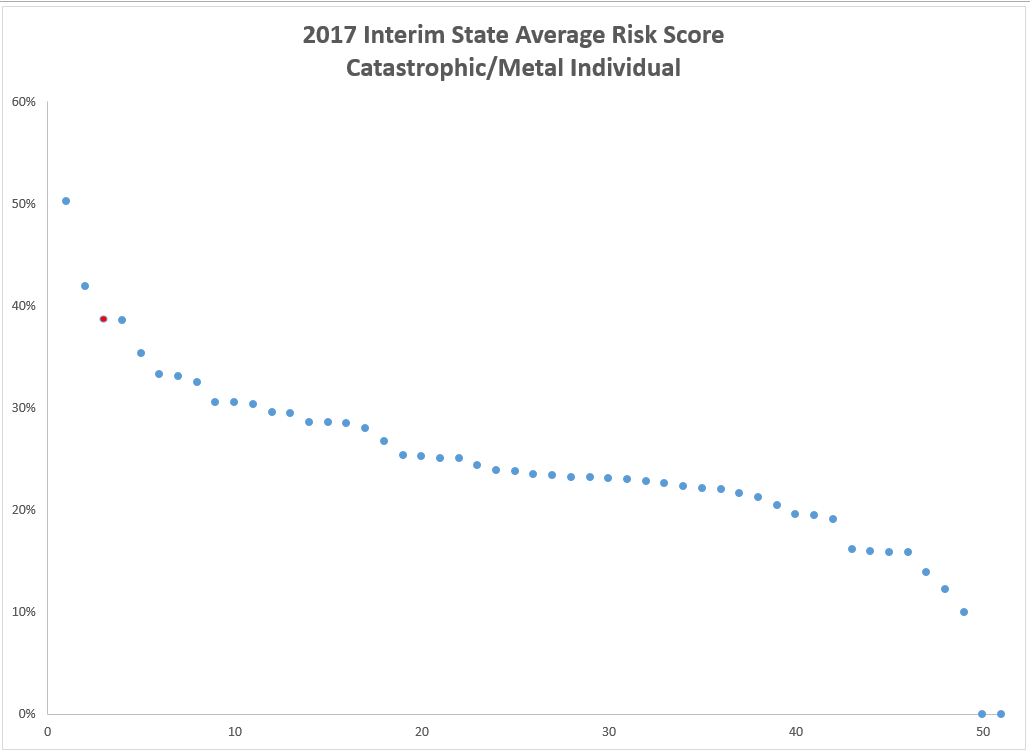
I think I am wrong. This rule has some pragmatic impact as it will worsen the Metal risk pool’s morbidity as more people can now buy Catastrophic plans.
Yet another hole in the hull — Single carrier hardship exemptionPost + Comments (9)