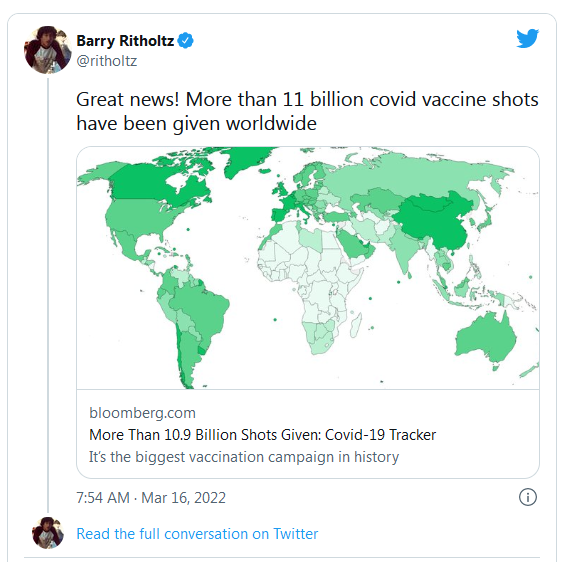
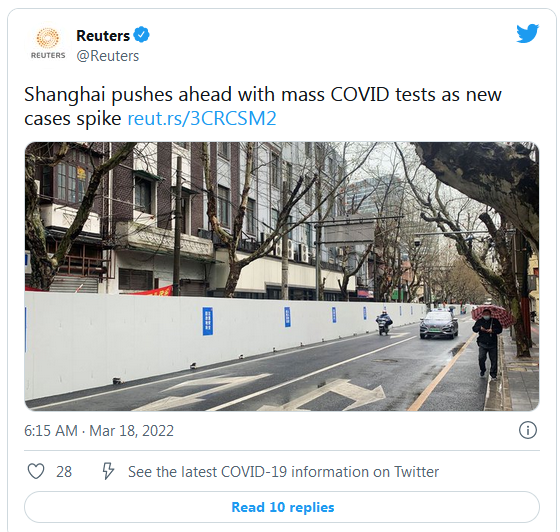
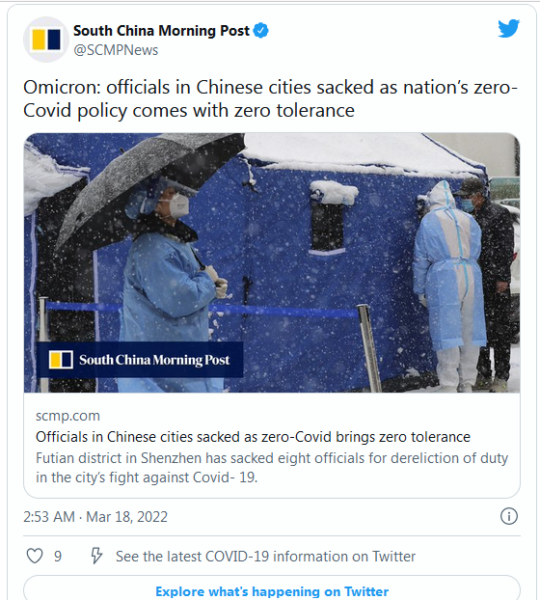
Across America, people have made tremendous sacrifices to get us to this point with #COVID19. We must safeguard our progress and ensure life-saving tools are available for ALL Americans. We can't afford to stop here. 2/2
— Dr. Vivek Murthy, U.S. Surgeon General (@Surgeon_General) March 18, 2022
Dr. Jha’s been on the local news several times a week since the pandemic began. He’s been good at explaining every twist and complication over the last two years, and very good at projecting calm and optimism. Seems like the right choice for our current pandemic moment:
President Biden’s COVID-19 coordinator and his deputy will be replaced by Dr. Ashish Jha, the dean of the Brown University School of Public Health. Jha’s appointment comes as the White House shifts its strategy as the nation learns to live with COVID-19. https://t.co/7N6H8vc0af
— The Associated Press (@AP) March 17, 2022
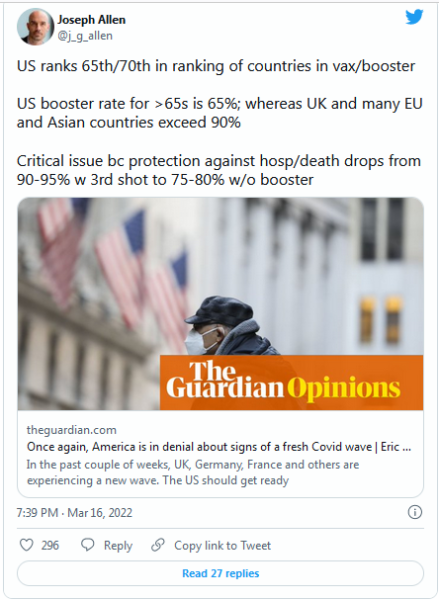
… When I first wrote about the panic-neglect cycle five years ago, I assumed that it would operate on a timescale of years, and that neglect would set in only after the crisis was over. The coronavirus pandemic has destroyed both assumptions. Before every surge has ended, pundits have incorrectly predicted that the current wave would be the last, or claimed that lifesaving measures were never actually necessary. Time and again, neglect has set in within mere months, often before the panic part has been over. The U.S. funds pandemic preparedness “like Minnesota snow,” Michael Osterholm, an epidemiologist at the University of Minnesota, told me in 2018. “There’s a lot in January, but in July it’s all melted.”
Or, as it happens, in March.
This week, Congress nixed $15 billion in coronavirus funding from a $1.5 trillion spending bill, which President Joe Biden then signed on Tuesday. The decision is catastrophic, and as the White House has noted, its consequences will unfurl quickly. Next week, the government will have to cut shipments of monoclonal-antibody treatments by a third. In April, it will no longer be able to reimburse health-care providers for testing, vaccinating, or treating millions of uninsured Americans, who are disproportionately likely to be unvaccinated and infected. Come June, it won’t be able to support domestic testing manufacturers. It can’t buy extra doses of antiviral pills or infection-preventing treatments that immunocompromised people are banking on but were already struggling to get. It will need to scale back its efforts to improve vaccination rates in poor countries, which increases the odds that dangerous new variants will arise. If such variants arise, they’ll likely catch the U.S. off guard, because surveillance networks will have to be scaled back too. Should people need further booster shots, the government won’t have enough for everyone…
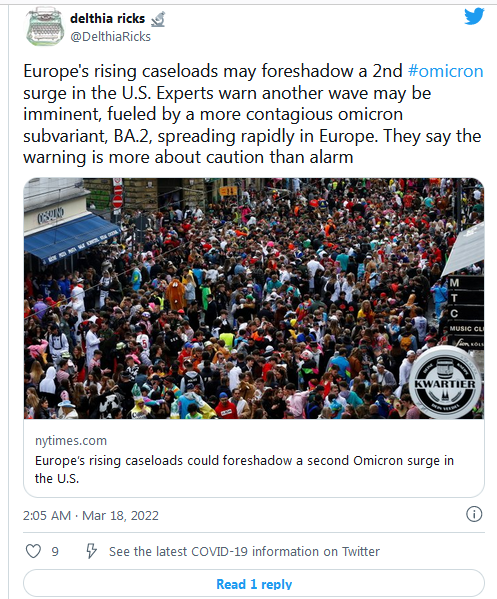
The virus is moving too. Cases are shooting up across Western Europe, auguring a similar rise in the U.S., as has happened in every past surge. (A third of the CDC’s wastewater sites have detected upticks in coronavirus samples this month, although such data are noisy and hard to interpret when levels of virus are low.) Meanwhile, mask and vaccine mandates are being lifted. Contact tracing and quarantine policies are being discontinued. The CDC’s new guidelines recast most of the country as “low risk” and left the most vulnerable individuals with the burden of protecting themselves. Some experts supported the guidelines on the grounds that testing, treatments, and other defensive tools were available—and, as promised in Biden’s recently unveiled national plan, would be strengthened even further. But those promises were always contingent on congressional funding; without it, those residual layers of protection evaporate too. For half a year, Biden, administration officials, and several prominent public-health voices have encouraged optimism because “we have the tools” to fight the virus. The first half of that catchphrase now seems doubtful…
… The virus is invisible. The ruin it inflicts is hidden from public view. The pandemic has gone on for two long years, turning tragedy into routine and breeding fatalism from failure. Older, disabled, poor, Black, or brown Americans, whose excess deaths were tolerated long before COVID, have borne the brunt of the pandemic, while privileged people have had the swiftest access to medical interventions—and have been quickest to declare the crisis over. A country that so readily forgets its dead is surely prone to also forgetting the lessons of the all-too-recent past, setting itself up for further failure in an all-too-imminent future.
======
… The U.N. health agency has previously said that the acute phase of the pandemic could end this year but it would depend on how quickly we meet its target to vaccinate 70% of the population in each country, among other factors.
Asked by a journalist at a Geneva media briefing about the timing of the pandemic’s end, Margaret Harris said it was “far from over”. “We are definitely in the middle of the pandemic,” she added.
After more than a month of decline, COVID cases started to increase around the world last week, the WHO said, with lockdowns in Asia and China’s Jilin province battling to contain an outbreak.
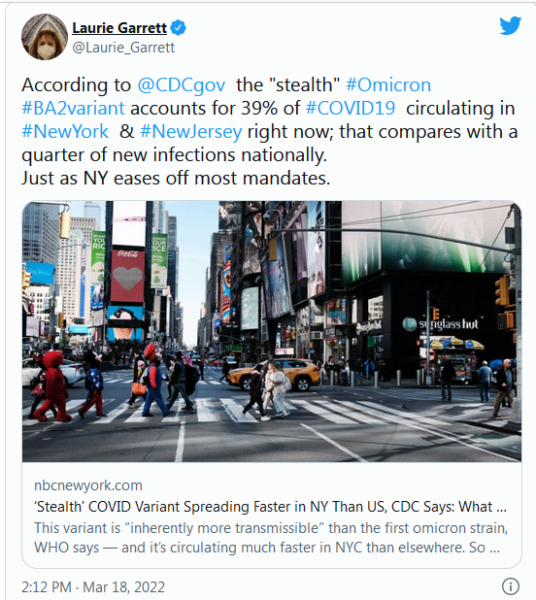
A combination of factors was causing the increases, including the highly transmissible Omicron variant and its cousin the BA.2 sub-variant, and the lifting of public health and social measures, the WHO said.
Mainland China reported its first COVID-19 deaths in more than a year on Saturday, according to a post on the National Health Commission's website that said two people died in the northeastern region of Jilin. https://t.co/jL1AhDIVqx
— Reuters Health (@Reuters_Health) March 19, 2022
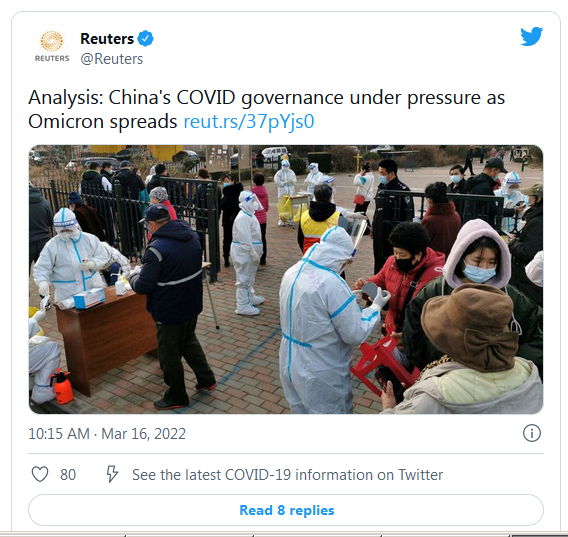
How does China exit the pandemic? We know it's tricky, but this time, its the officials raising it publicly. this is even as omicron drives a surge in Hong Kong and the mainland w/ @dakekang — https://t.co/AFQwsg4U9l
— Huizhong Wu (@huizhong_wu) March 18, 2022
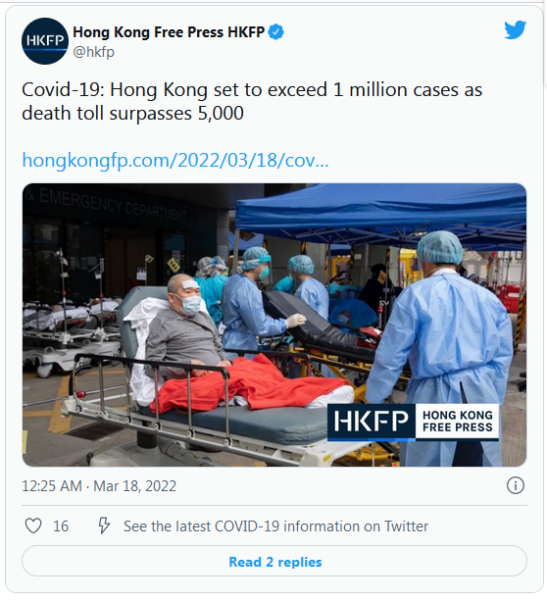
Hong Kong reported 16,597 Covid-19 infections on Saturday, of which 9,069 were from rapid tests. The city added another 249 deaths, including 61 from backlogs and 6 who died before reaching the hospital. pic.twitter.com/oWs1yf9r4p
— Hong Kong Free Press HKFP (@hkfp) March 19, 2022
As Hong Kong residents leave the city, in part due to the city's tough COVID rules, many chose to abandon their pets, overwhelming dog shelters, which are running at full capacity https://t.co/rHy7NnPGyP pic.twitter.com/EK5R88q5BA
— Reuters (@Reuters) March 18, 2022
So. Korea’s coronavirus infections have soared to one of the world’s highest w/ an #omicron-fueled surge. Thursday S. Korea recorded its deadliest day of the pandemic: 429 deaths in 24 hrs. Officials reported >621k cases, ~1% of the entire population https://t.co/GK45qis30q
— delthia ricks ? (@DelthiaRicks) March 18, 2022
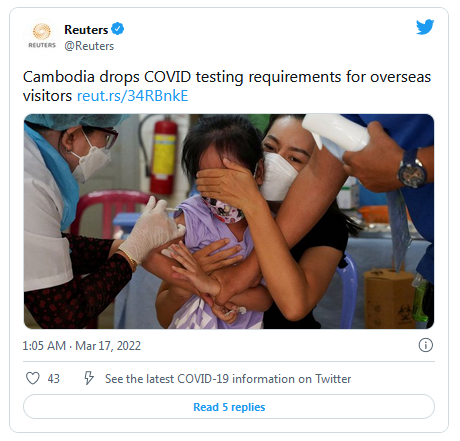
Ecuador’s president on Friday announced an end to coronavirus limits on public and private gatherings, but the South American country will continue to require foreign visitors to show proof of vaccinations or a negative COVID-19 test.
President Guillermo Lasso said the government made the decision to end two years of pandemic containment measures because Ecuador has reached its goal of fully vaccinating 85% of the population above five years old.
Both new infections and COVID-related deaths have steadily fallen in recent weeks, according to government data…
Lasso’s government is maintaining for the time being rules requiring face coverings in all public spaces, including outdoors, as well as indoor spaces…
According to health ministry data, about 583,000 coronavirus infections have been confirmed over the past two years, along with some 35,000 deaths, which officials describe as the sum of both confirmed and probable fatalities.
Only about 30% of Ecuador’s adult population have received booster shots and the government only recently began vaccinating three- and four-year-olds.
======
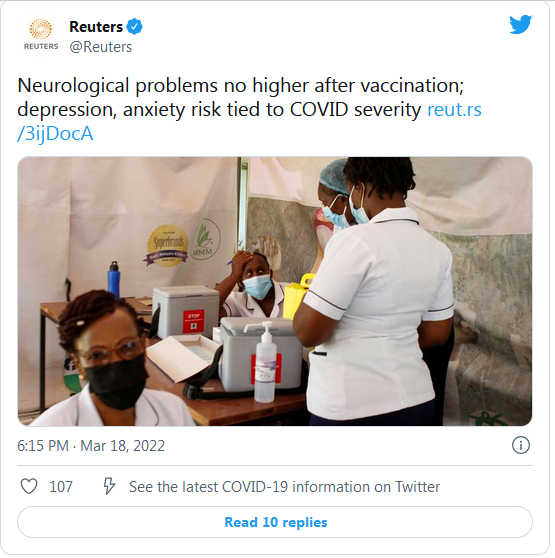
… COVID-19 vaccination did not increase risks for rare neurological conditions among more than 8 million people who had received at least one dose of a vaccine from AstraZeneca (AZN.L), Pfizer /BioNTech (22UAy.DE), Moderna (MRNA.O) or Johnson & Johnson (JNJ.N), according to researchers.
Their study also included 735,870 unvaccinated individuals who had tested positive for the coronavirus, as well as older data on an additional 14.3 million people from the general population for a baseline estimate of rates of the neurological conditions before the pandemic. Researchers looked for four neurological disorders involving the immune system. Three of them – Bell’s palsy (facial weakness), encephalomyelitis (inflammation of the brain and spinal cord), and Guillain-Barré syndrome (a nerve condition) – were no more common in the vaccine recipients than in the general population, the researchers reported on Wednesday in The BMJ. The fourth – transverse myelitis (inflammation of the spinal cord) – occurred too rarely for analysis (fewer than 5 cases in 8.3 million vaccinated people). The researchers did see increased rates of Bell’s palsy, encephalomyelitis and Guillain-Barré syndrome in COVID-19 survivors, however…
Risk of depression, anxiety tied to COVID-19 severity
People who have been bedridden for seven days or more with COVID-19 are at increased risk of anxiety and depression, an international study found.Researchers analyzed data from Denmark, Estonia, Iceland, Norway, Sweden and the UK collected between March 2020 and August 2021 on more than 247,000 people, including 9,979 who were diagnosed with COVID-19. Those who had COVID and were bedridden for at least a week had a 61% higher risk for symptoms of depression and a 43% higher risk for anxiety, for up to 16 months after their diagnosis compared to those who were never infected.
By contrast, patients who had COVID-19 but were never bedridden actually had significantly lower rates of depression than people who had never contracted the virus, researchers found. “This group may experience a relief after recovery from the relatively benign infection and are able to return to somewhat normal lives as compared to those not yet diagnosed with COVID-19, perhaps still fearing infection and therefore still limiting social contact,” said Dr. Anna Valdimarsdottir of the University of Iceland, whose team reported the findings in The Lancet Public Health. The results should alert clinicians to the possibility of long-term mental health symptoms in their patients who suffered severe acute illness from the virus, she added.
Imp. paper in the world’s best biomedical journal. Not great news for natural omicron infection doing as much as hoped to contribute to the ‘wall of immunity’. You’re NOT bullet proof if previously infected. Everyone – get your 3rd dose & avoid infection as best you can. #COVID19 https://t.co/xC7l7S7o7g
— Prof Brendan Crabb (@CrabbBrendan) March 18, 2022
======
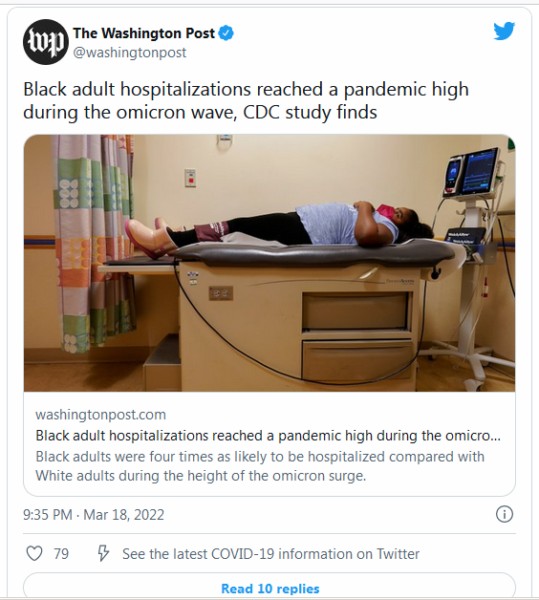
In D.C., Maryland and Virginia, one of the most vaccinated regions in the country, 7,100 people have died of covid-19 since Christmas https://t.co/Iqhm8paJVu
— The Washington Post (@washingtonpost) March 18, 2022
People shrug over flu. Will they soon be shrugging about Covid? https://t.co/xXxgr7yGrI
— delthia ricks ? (@DelthiaRicks) March 18, 2022
COVID-19 Coronavirus Updates: Friday / Saturday, March 18-19Post + Comments (15)